Why Certain Small Dogs Shouldn't Wear Collars
A serious, yet often hidden condition that can develop over time - it can leave your dog feeling like she's trying to draw in air through a flattened straw. Obesity, anesthesia, collars, air fresheners and scented candles can make the condition worse. These supplements may help stave it off.
STORY AT-A-GLANCE
- Tracheal collapse is a significant, chronic, and progressive disease that affects breathing and quality of life; the condition is most often seen in small breed dogs
- The disease can be genetic or can develop over time; dogs with the condition should not be bred to avoid passing it on to future generations of puppies
- The first sign of tracheal collapse is often a dry cough; as the disease progresses, additional symptoms may develop such as exercise intolerance and difficulty breathing
- Mild cases of tracheal collapse can often be successfully managed with a multimodal treatment approach; in severe cases that can't be medically managed, surgery may be the best or only satisfactory option
- Dogs with the condition do best in a very clean, nontoxic environment and also benefit from cartilage-building supplements; they should also wear a harness instead of a collar
Editor's Note: This article is a reprint. It was originally published April 04, 2022.
Tracheal collapse is a potentially very serious disorder that primarily affects small dogs. The condition can be present at birth (congenital) or develop later in life (acquired).
The trachea is the scientific name for the windpipe, which is the tube that connects the nose, mouth, and throat to the lungs. When a dog inhales, the diaphragm, which is the flat muscle that separates the abdomen from the chest cavity, flattens and the muscles between the ribs move to pull air into the lungs. When he exhales, the muscles move in the opposite direction to push air out of the lungs. The trachea enables the passage of air in and out of the lungs.
Part of the trachea is in the throat, and a portion also extends down into the chest. It looks a bit like a vacuum cleaner hose and is made of muscle connected by small rings of cartilage that keep the tube open. These rings are C-shaped, with the open part facing upward toward your dog's back. Running along the top opening of the C-rings is a band of tissue called the dorsal tracheal ligament, also referred to as the tracheal membrane or the dorsal membrane.
The C-rings that give the windpipe its round shape can weaken over time, changing it from a C-shape to more of a U-shape. In some dogs, the rings of cartilage are misshapen at birth.
Congenital Tracheal Collapse
When the condition is congenital (present at birth), it's typically the result of an inherited deficiency in certain components of the cartilage rings, like calcium, chondroitin, glycoproteins and glycosaminoglycans (glucosamine).
If you're considering buying a puppy with a breed predisposition to this disorder, it's important to know that currently, there's no test to check for the condition. I recommend calling your breeder's references to see if any dogs in your prospective puppy's lineage have the problem.
Fortunately, responsible breeders focus on breeding for reparative conformation, meaning they take steps to try to breed exaggerated features and specific inherited health problems out of future litters. Ethical breeders of small dogs will choose to not to breed animals with a history of tracheal collapse.
Since there are lots of irresponsible breeders out there just looking to make a buck, along with uninformed breeders, you can help by refusing to buy puppies from pet stores (almost all of which get their animals from puppy mills). The majority of these retailers and puppy mill operators don't care what health problems the dogs have or may develop over time.
If you're planning to invest money in a puppy of a breed prone to tracheal collapse, find a breeder who can explain to you what he or she is doing to prevent litters of puppies with an inherited tendency to the condition.
Acquired Tracheal Collapse
A collapsing trachea can also develop over time, and is often caused by chronic respiratory disease, Cushing's disease, or heart disease. Whether congenital or acquired, the weakened C-rings cause the ligament along the top of the windpipe to loosen.
Instead of a tight canopy-like structure running along the top of the trachea, the membrane becomes lax and floppy. As the cartilage rings get progressively flatter, eventually the trachea collapses either along its entire length, or only in the portion that resides in the throat. Most often, the collapse is worse in the area where the trachea enters the chest.
Once this happens, the poor dog is left trying to draw air through what is essentially a flattened straw. Panting or rapid breathing makes the collapse worse, which leads to more rapid breathing as the dog's anxiety increases. The condition also triggers inflammation in the trachea, which over time causes tissues to change and lose their normal characteristics, further aggravating the condition.
Risk Factors and Symptoms
Tracheal collapse is most often seen in toy breeds, especially toy poodles, Yorkshire terriers, and Pomeranians. This condition typically becomes a problem when a dog reaches middle age, but it can occur at any age.
Many dogs with tracheal collapse have no obvious symptoms until a secondary problem arises. Factors that can trigger tracheal collapse include:
- Obesity
- Kennel cough or another respiratory infection
- An enlarged heart
- Environmental respiratory irritants, such as cigarette smoke, dust, or other airborne toxins such as air freshener sprays and plug-ins, and scented candles
- Delivery of anesthesia that involves inserting an endotracheal tube
One of the first signs of tracheal collapse can be a sudden attack of dry coughing that sounds a little bit like a goose honk. Typically, the goose honk sound progresses to more of a consistent cough, and often occurs when there's pressure placed on the trachea. This can happen when a dog is picked up or when his collar is being pulled against his neck.
As the disease progresses, the dog can develop exercise intolerance, obvious respiratory distress, and gagging while eating or drinking. Some dogs with tracheal collapse turn blue when they're excited or stressed.
Secondary heart disease can result when a dog is constantly straining to breathe. In addition, some dogs have both laryngeal paralysis and tracheal collapse. These dogs usually make a wheezing sound when they breathe in.
Diagnosing Tracheal Collapse
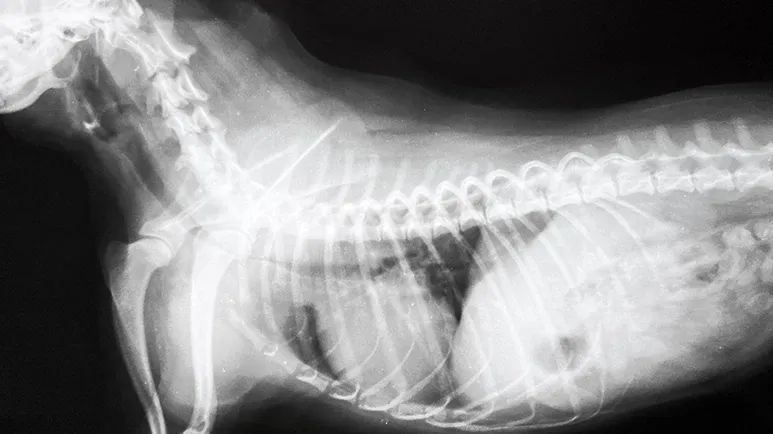
Tracheal collapse can sometimes be seen on a standard X-ray as a narrowing of the tracheal lumen. Fluoroscopy, which is a moving X-ray, allows your veterinarian to watch your dog's trachea as he breathes in and out.
An endoscopy, in which a camera is passed down to your dog's trachea, allows a view inside the organ. During this procedure, your veterinarian can also take samples of the trachea for culture and sensitivity tests or additional analysis. Sometimes an echocardiogram is recommended to evaluate heart function.
Any disease of the upper or lower airway can be mistaken for tracheal collapse, including a foreign object in the respiratory tract, laryngeal paralysis, an elongated soft palate, an infection of the trachea or lungs, heart failure, and tumors or polyps. It's very important that your veterinarian rules out all other potential causes for your dog's symptoms before arriving at a diagnosis of tracheal collapse.
Treatment and Condition Management
Conventional medical treatment of mild to moderate cases of tracheal collapse typically involves the use of cough suppressants, antispasmodics, bronchodilators, and calming agents to help reduce coughing spasms and the associated anxiety.
It's important to interrupt the coughing cycle because coughing irritates the airway and leads to more coughing. The earlier we can intervene with natural cough remedies, the better. I often use several different remedies, including a cool tincture of slippery elm, licorice root, mullein, or wild cherry bark teas and organic honey, all of which can help suppress the cough.
If a secondary factor is triggering or exacerbating a collapsed trachea, often resolving that issue (treating a respiratory infection, for example, or getting your dog's weight under control) will also help reduce the symptoms of collapsing trachea.
In addition, I recommend that you check your dog's environment for potential triggers, such as smoke (of any kind) and other environmental pollutants. Get rid of flame-retardant (PDBE) treated dog beds and invest in a nontoxic pet bed made with all-natural fibers. Switch to organic household cleaners and throw out your plug-ins, scented room sprays, and scented candles. Consider getting a room air purifier.
Any dog with a collapsing trachea should be walked using a harness only, never a collar (or a bandana, or turtleneck coat or sweater, or anything around the neck at all), as reducing all pressure on the throat is critical. Traditional collars can dramatically exacerbate tracheal collapse because they apply constant pressure to the trachea.
Beneficial Supplements
Medical management and trigger elimination works for about 70% of dogs with mild tracheal collapse. I and most integrative veterinarians also recommend cartilage builders to help maintain the integrity of the tracheal cartilage.
The earlier you begin these trachea-supporting supplements, the better. If your dog has a genetic predisposition to the condition, I recommend beginning supplementation at six months of age and continuing cartilage support for a lifetime. This proactive approach can radically reduce the expression and progression of this degenerative disease. These supplements can include:
- Glucosamine
- Perna mussel (green lipped mussel)
- Chondroitin
- Methylsulfonylmethane (MSM), which is an important source of organic sulfur, a main constituent of healthy cartilage
- Eggshell membrane
- Cetyl myristoleate (CMO)
- Collagen (sourced from grass-fed animals)
Many dogs also benefit from organic trace mineral supplementation or whole-food sources of silica, manganese, and magnesium, as well as supplemental vitamin C. Natural anti-inflammatories such as proteolytic enzymes and turmeric can also be beneficial in reducing tracheal inflammation. In addition, cannabidiol (CBD) oil can be very useful in alleviating symptoms, including anxiety.
In some dogs, chiropractic treatments and acupuncture have helped reduce the intensity and duration of coughing episodes, and both homeopathy and Chinese medicine may help with this condition as well.
A Word About Surgery for Tracheal Collapse
In my opinion, surgery for tracheal collapse should be avoided except in life-threatening situations. It should be reserved for only the most severe cases of collapsing trachea in dogs who don't respond to medical management.
If the collapse is happening in the neck or the thoracic inlet, plastic rings are placed surgically around the inside of the trachea. If the collapse is deeper in the chest, a stent — a tiny spring that holds the trachea open — is placed.
Stent placement achieves improvement in clinical signs in most dogs, but unfortunately, complications are common within a few years and may require placement of a second stent.
Surgical repair of a collapsing trachea is a very specialized procedure with significant potential for complications. These procedures should only be performed by a veterinary surgeon with extensive knowledge and a well-equipped hospital with a staff capable of helping your dog recover in an appropriate manner.
I really recommend avoiding this surgery unless you've exhausted all forms of therapy and your dog's ability to move oxygen is affected, potentially becoming a life-threatening situation. Thankfully, these cases are relatively rare.
Tracheal Collapse and Liver Disease
A study published in 2006 suggests liver disease may go hand-in-hand with a collapsing trachea.1 Researchers looked at 26 dogs with tracheal collapse and compared their liver function tests with 42 dogs with normal tracheas. Most dogs with tracheal collapse — 92% — had abnormal liver function test results.
When some of the dogs received tracheal stents to alleviate symptoms, their liver values improved. The researchers concluded oxygen deprivation from a collapsing trachea may impact liver health, and therefore, liver function should be routinely assessed in dogs with collapsing trachea syndrome or another serious respiratory disease. I recommend this as well.
Tracheal collapse can be a very frightening and frustrating disease for pet parents. Dogs whose condition can be successfully medically managed have a good prognosis for a normal quality of life. The outlook for dogs with severe disease or who undergo stent placement is less optimistic.
If your dog has a collapsing trachea, her distress can become so severe that her normally pink, healthy-looking mouth and mucous membranes can turn a bluish color, and she can collapse. If your dog is in extreme distress or collapses, it's a medical emergency and she should be taken immediately to your veterinarian or the nearest emergency animal hospital.
The best option if your dog is dealing with a collapsing trachea, is to slow down the progression of the disease by being proactive. I recommend beginning a cartilage support protocol in high-risk breeds at around three years of age to help prevent tracheal cartilage deterioration.
Your second-best option is to address the problem at the very first symptom, before the disease progresses any further.













